Stepping Up the Fight Against Infant and Maternal Mortality
Among the world’s developed countries, the United States holds the unwanted distinction of being a leader in maternal and infant deaths. In an attempt to turn the tide, the federal government last month announced a new $350 million investment.
What Will It Take to Increase Maternal Vaccination Rates?
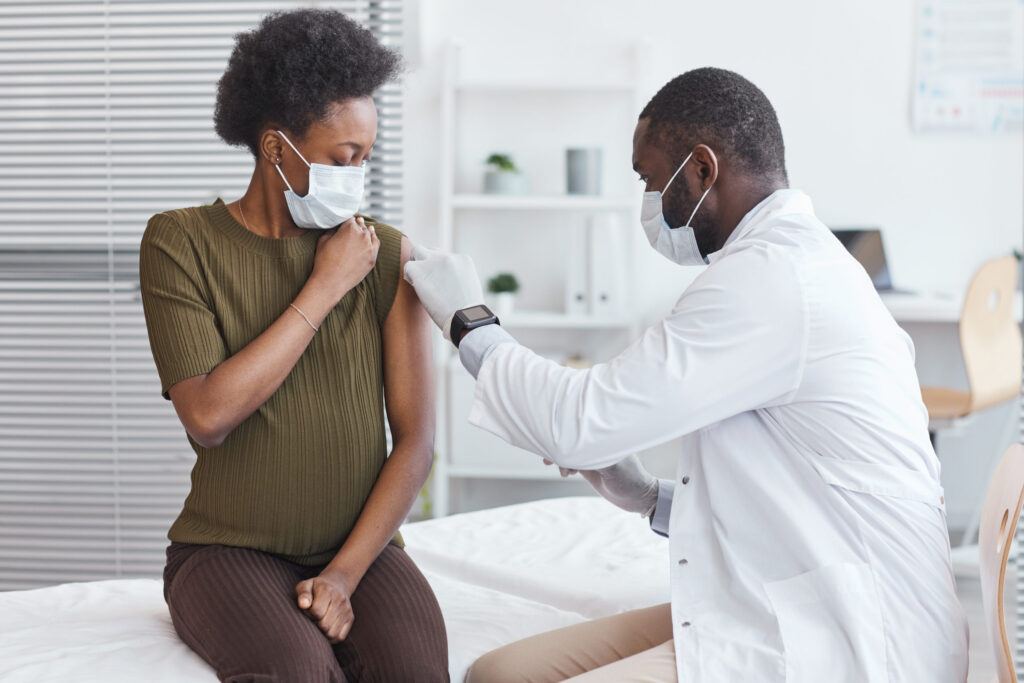
Maternal vaccines can protect pregnant moms and vulnerable babies. So why aren’t more women getting them?
Infant Health Policy Summit

The sixth annual Infant Health Policy Summit welcomed health care providers, parents, policymakers, advocates and other stakeholders to explore how policy solutions can improve the health and lives of infants and their families.
Summer Brings Unusual Spike in Children’s Respiratory Virus

Warm summer months usually provide a break from respiratory syncytial virus. But not this year.
From Mom to Baby: Antibodies and Infant Health

Everyone knows children inherit some things from their parents: their blue eyes, their curly hair, or perhaps their love of the outdoors. Moms take prenatal vitamins and get maternal vaccines like Tdap to transfer health benefits and good antibodies to their unborn babies.
For Newborns & Infants in the NICU, COVID-19 Restrictions May Do More Harm than Good

Babies born during the pandemic will never know what life was like “before 2020.” Yet policies meant to minimize the spread of COVID-19 may have a lifelong impact on babies born last year.
Black Maternal Health Crisis Captures White House Attention

America’s maternal mortality rates are among the highest in the developed world. It’s a crisis of epic proportions. And like many other crises, not all Americans are equitably affected.
Securing Babies’ Access to Life-Saving Medicine
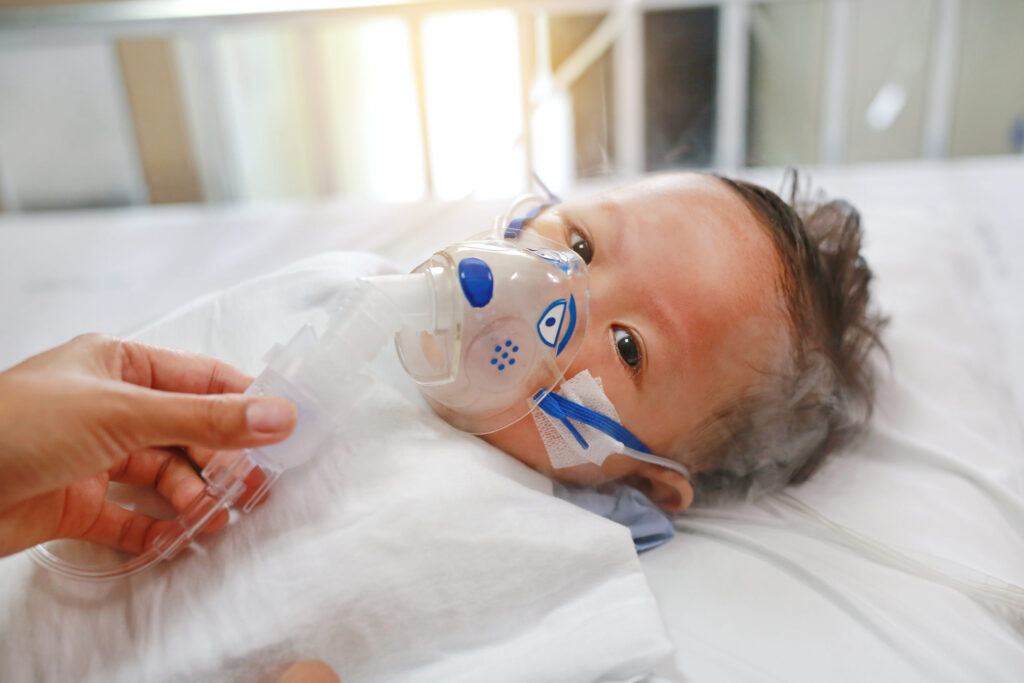
Bringing a newborn baby home from the hospital is a joy like no other. Bringing that same baby back to the hospital for treatment of a life-threatening virus would be a nightmare. Yet for tens of thousands parents, RSV makes that traumatic return trip a reality.
When Preterm Infants Struggle to Feed
Working in the NICU, I have observed a wide range of challenges affecting late preterm infants. But perhaps the most concerning is difficulty eating.
Human Milk: The Best Medicine for Vulnerable Babies
It fosters brain development. It passes on antibodies. It lowers the risk of infection. Human milk has long been known to offer many benefits to babies, especially to those born prematurely.

